
Arcadia Healthy Smiles
Services
We provide virtually every dental service available for your oral health. In the event that we feel the procedure you require is outside the of scope of our expertise, we will refer you to a specialist who is better able to meet your needs. After the specialist has completed the recommended treatment for you, our office will be ready to handle your follow-up care.
Cleaning and Prevention
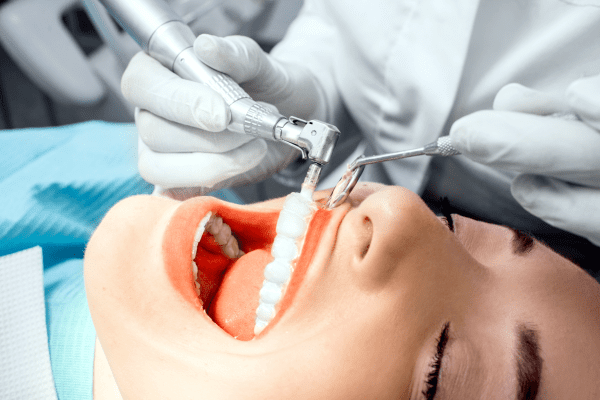
A preventive (recall) program is a joint cooperative effort between you and our team to preserve your natural teeth, gums, and bone of the oral area by preventing the onset, progress, and recurrence of dental diseases and conditions.
Preventing dental disease starts at home with good oral hygiene and a balanced diet. It is continued in our dental office by the efforts of Dr. Tran and the dental hygienists as they promote, restore, and maintain your oral health.
Regular dental exams, cleanings, and x-rays are all part of an effective prevention program. Other great preventive treatments include sealants and fluoride.
Prevention is needed to avoid serious and costly dental problems and is the key to having a healthy, confident, and beautiful smile.
Gum and Bone

Periodontics is that specialty of dentistry that encompasses the prevention, diagnosis and treatment of diseases of the supporting and surrounding tissues of the teeth. This includes crowns, implants, or other substitutes and the maintenance of the health, function and aesthetics of all of the structures and tissues.
Professional dental cleanings are necessary at least twice each year to maintain good oral health. Many people require a routine cleaning three or four times a year due to buildup of plaque and tartar.
If you have been told you have periodontal (gum) disease, you’re not alone. An estimated 80 percent of American adults currently have some form of the disease.
Periodontal diseases range from simple gum inflammation to serious diseases that result in major damage to the soft tissue and bone that support the teeth. In the worst cases, teeth are lost.
Gum disease is a threat to your oral health. Research also points to possible health effects of periodontal diseases that go well beyond your mouth (more about this later).
Whether it is stopped, slowed, or gets worse depends on how well you care for your teeth and gums every day.
Oral Surgery

Oral and maxillofacial surgeries are special areas of dentistry concerned with the diagnosis and surgical treatment of congenital or acquired diseases; dysfunction, defects, or injuries of the mouth, jaws, face, neck, and associated regions.
Some of these issues are:
When Teeth Are Lost
When a tooth must be extracted due to trauma, bone loss, or other reasons, implants may be placed in the bone if your dentist determines that you area a good candidate for implants.
Impactions
The wisdom teeth, or third molars, are the most frequently impacted teeth due to lack of space in the jaw. In most cases, wisdom teeth that do not erupt into proper alignment should be extracted. Please visit our wisdom teeth page to see the different types of impactions.
Jaw Alignment
Oral surgery can correct cases where the jaw bones are under- or overdeveloped. Cases where the upper jaw grows either too much or too little and/or the lower jaw grows too much or too little can be surgically corrected and realigned.
TMJ – Temporomandibular Joint
Otherwise known as the TMJ, this joint in front of the ear where the lower jaw pivots is a common problem area. Problems with this joint can cause headache and continuous pain. Lesser cases can be corrected with medication, therapy, and splints. However, more serious cases may require reconstruction of the joint.
Biopsy
When there is a suspicious growth or changed appearance of a section of tissue in the mouth, a biopsy will be performed to determine the origin of the lesion.
Facial Trauma
Oral surgery can help in cases of facial trauma that results from accidents or facial genetic malformation of the jaw and face.
Orthodontics

Orthodontic treatment corrects teeth and jaw alignment problems and involves the design and use of appliances such as braces, retainers, aligners, rubber bands, and headgears. If you have crowded or overlapping teeth, it makes them harder to clean which increases your chances of tooth decay, gum disease, and eventual tooth loss. With orthodontic treatment, you can improve the health of your teeth and start to smile with confidence!
Early intervention and treatment is preferred, since the process is usually quicker and easier. Treatment can begin as early as six or seven, which is when some habits that are formed as a baby can begin to cause unwanted tooth movement. Orthodontic treatment is also available for adults, who can be treated with both fixed and removable appliances.
Pedodontics

Pediatric dentistry is the branch of dentistry that deals with infants, children and adolescents including those patients with special care needs.
Do you have to be a pediatric dentist to treat children?
No you don’t. However, a pediatric dentist attends a post graduate program after dental school for two to three years to learn more about the specific needs of young dental patients.
Do I need to brush my children’s teeth?
Yes because children develop plaque just like adults do and it must be removed on a daily basis so it does not lead to tooth decay. Use a soft-bristled toothbrush that will fit into the child’s mouth at least once a day to begin with when they are very young and at least twice a day by the time most of the baby teeth have erupted.
When should I take my child to the dentist for the first time?
You should schedule an appointment around the first birthday so that we can check for good oral hygiene, cavities and any developmental or congenital abnormalities.
If baby teeth eventually fall out, why are they important?
Baby teeth are very important because they serve many of the same purposes of adult teeth such as tearing and chewing food and helping the child speak properly. Additionally, they hold the place for adult teeth. If baby teeth are lost prematurely, an appliance called a space maintainer is needed to prevent the remaining teeth from shifting into the space of the lost tooth.
How do thumb sucking and pacifier habits harm teeth?
There is not much difference between the two habits and they only become a problem if the baby teeth start to get displaced or if the habit continues after the adult teeth have erupted. Read more here about thumb sucking and pacifiers.
I did not give my baby candy but he still has decay. How can that happen?
Decay is not only caused by candy; it can be caused by most foods or liquids other than water that do not get removed from the surface of teeth. Infants and children are at the mercy of their parents. If a toddler is continuously given a bottle with almost anything other than water at bedtime, they will probably develop baby bottle caries, which are cavities on the front teeth. Do not give a bottle with anything other than water at bedtime and get in the habit of brushing your child’s teeth on a regular basis.
How often do children need to visit the dentist?
Children should visit a dentist every six months. We like to catch anything when it is small and seeing the child every six months gives us the best chance to keep an eye out for any signs of early decay. Additionally, since teeth start coming and going, we like to have a history of each patient’s dental development.
Is toothpaste good or bad for children?
Fluoridated toothpaste should not be used for children under age 2. After that time, parents should be in charge of dispensing the toothpaste and the amount to be used each time should not be bigger than the size of a pea. Make sure the children spit the toothpaste out instead of swallowing it. It is not dangerous if they swallow it once or twice but do not let it become a habit.
Should baby teeth be sealed?
Baby teeth should be sealed if they have deep pits and fissures that may be prone to decay without a sealant.
Cosmetic Dentistry
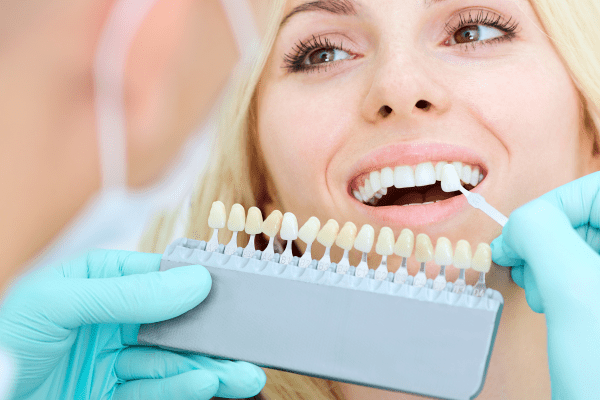
There are many reasons why adult teeth may need restorative treatment. The most common reason is decay, followed by fractured teeth, and old restorations needing replacement. If we recommend that a tooth with a cavity be treated and more than a few weeks pass after the initial diagnosis, the cavity will almost always get bigger and can cause pain. Once this happens, it will likely require more extensive and expensive treatment. The tooth may even have to be removed and replaced with a false (or artificial) tooth. If you have a cavity and it needs a restoration, there are different kinds of materials that may be used to restore the functionality of the tooth. Please remember that a tooth may need treatment before it causes pain. If a tooth causes pain, it may be able to be saved, but the treatment time and cost typically increase due to the complexity of the necessary procedures.
How a Cavity Forms
A cavity is a very small hole that forms on the surface, side, or root of a tooth. Cavities are caused when sugars in the food you eat combine with the bacteria in your mouth. This combination produces a mild acid that eats away at the enamel, the hard outer layer of your tooth. Cavities can occur at any age, but most occur during childhood when dental hygiene may be less thorough. There is a genetic component to dental health, including teeth, gums, and the bone that holds the teeth. No matter how good your genes are, if you don’t take good care of your teeth you may be prone to very serious consequences.
Babies tend to get cavities on the front teeth, especially if they are given a bottle to sleep with. Even milk contains sugar that can harm teeth. This is referred to as baby bottle tooth decay. Children tend to get cavities on the chewing surfaces as well as in-between teeth. Adults can be at risk for both new and recurrent cavities.New cavities tend to form between teeth as well as on the root surfaces. The cavities that form between teeth are typically related to a lack of flossing. Cavities on the root surfaces of teeth generally occur because this area is not covered with enamel and is softer and more prone to cavities. The exposed root may be the result of hard brushing or bone loss related to gum disease. Cavities that reoccur form next to existing restorations such as fillings, crowns, bridges, etc. As restorations get old, the filling material can shrink or wear away, causing the possibility of a small space forming between the tooth and the restoration. This provides a prime area for bacteria to accumulate and breed decay. Click the link to do an experiment with fluoride to see how it helps fight cavities.
Cavities and Restoration Choices
As part of any visit to our office, we check all of your restorations such as crowns, fillings, bridges, veneers, etc. for any sign of decay or old age and we may recommend x-rays so that we can see inside and between your teeth. If we spot any cavities, we will recommend different options for restoring the tooth to full function. If the cavity is in the very early stages, we may decide to keep an eye on it and recommend a home fluoride rinse to help the tooth fight the cavity and possibly prevent the need for a restoration.
Root Canal
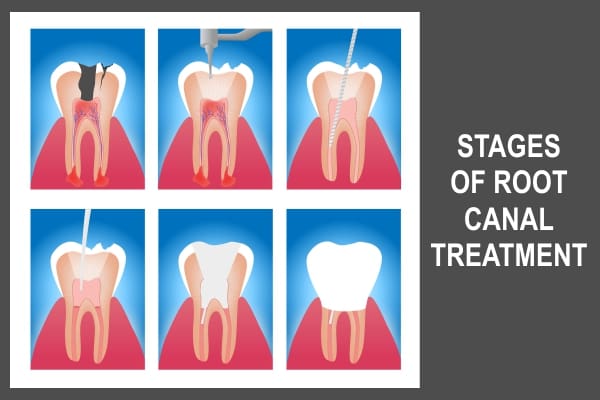
Endodontics (Root Canal Therapy)
The term endodontic is a combination of the Greek words endo, which means “inside” and odont, which means “tooth.” Endodontic treatment involves treating the inside of the tooth and is also referred to as root canal therapy because it is focused on the root part of the tooth, specifically in the canal portion of the root where the nerve, blood vessels, and connective tissue of the tooth reside.
Inside of a tooth, under the white enamel and a layer called the dentin, is soft tissue called the pulp. The pulp contains blood vessels, nerves, and connective tissue and creates the surrounding hard tissue of the tooth during development.
The pulp extends from the crown of the tooth to the tip of the roots where it connects to the tissues surrounding the root. The pulp is very important during a tooth’s growth and development. However, once a tooth is fully mature, it can survive without the pulp because the tooth continues to be nourished by the tissue surrounding it.
Why Endodontic Treatment is Necessary
Decaying tooth: Root canal therapy is necessary when the pulp becomes inflamed or infected. The inflammation or infection can have a variety of causes: deep decay due to bacteria, multiple dental procedures on the tooth, or a crack or chip in the tooth. In addition, trauma to a tooth may cause pulp damage even if the tooth has no visible chips or cracks. If pulp inflammation or infection is left untreated, it can cause pain, and/or lead to an abscess.
Signs of pulp damage may include pain, prolonged sensitivity to heat or cold, discoloration of the tooth, and swelling and tenderness in the nearby gums. Sometimes there are no symptoms at all.
Treating the Tooth
Root canal treatment: A traditional root canal involves removing the inflamed or infected pulp, carefully cleaning and shaping the canals inside of the tooth, then filling and sealing the space inside the canal. A crown holds the tooth together and reduces the likelihood of the tooth fracturing in the future. Back teeth often need crowns since a great amount of tooth structure may be lost from decay, which makes them more susceptible to fracture. Front teeth occasionally need crowns and are restored with a crown on a case-by-case basis.
Root Canal Procedures Explained
Endodontic treatment can often be performed in one or two visits, depending upon the source of the problem and the complexity of the tooth. The first step is to examine, test, and x-ray the tooth. The area is then numbed with local anesthetic to reduce or eliminate pain. Next, a rubber dam is placed to isolate the tooth from the rest of the oral cavity, creating a barrier to prevent bacteria and saliva from entering the tooth during the procedure. We then use a handpiece to open access into the pulp chamber and root canals. Very small instruments are used to clean and shape the pulp chamber and root canals to remove the nerve, blood vessels and connective tissue, and to prepare the canals for the root canal filling material.
Filling the Canals
After the space is cleaned and shaped, we fill the root canals with a biocompatible material which is placed with an adhesive cement to ensure the complete sealing of the root canals. The goal of the filling material is to create a barrier so that no cells, fluids, or other matter enters the tooth at the tip of the root. In some cases, a temporary filling is placed to prevent anything from entering the tooth from your mouth. It is important that this temporary is replaced by a final restoration in a short amount of time as it is not meant for long term wear.
Restoring the Tooth
Root canal tooth restoration: If the tooth lacks sufficient structure to hold a restoration after the root canal, a core build-up or post will need to be added inside of the tooth. This provides a solid foundation for a crown and fills the hollow space that was created to access the pulp and canals of the tooth. A crown or other restoration is then placed on the tooth to protect and restore it to its full function.
Sedation Dentistry
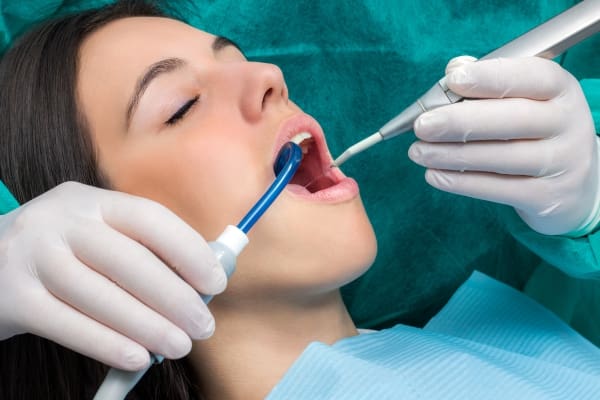
- Are dental fears keeping you from having a healthy mouth?
- Are you afraid of going to the dentist?
- Has it been a long time since your last dental appointment due to fear?
- Do you have sensitive teeth and gums?
- Are you immune to traditional methods of numbing techniques?
If you answered “yes” to any of these questions then conscious sedation is for you.
Who Benefits from Conscious Sedation?
- Anyone who has fear and anxiety about dental treatment of any kind.
- Anyone who has put off dental care for years because of dental anxieties.
- Anyone who wants to have all their dental care completed in one or two visits.
- Anyone who wants to be treated in a relaxed, caring and comfortable environment.
What To Expect
One hour before your appointment, you will take a pill. You will need a driver to escort you to and from the dental office. You will likely be drowsy upon arrival.
You’ll be sedated just enough to be unaware of the treatment, as if you were asleep. We can perform a wide range of dental procedures in a single visit.
Treatment Completion
Upon completion of your dental treatment under conscious sedation, you will feel relaxed with little or no memory of the procedure.
TMJ

TMJ – Temporomandibular Joint Information
Temporomandibular joint and muscle disorders, commonly called TMJ, are a group of conditions that cause pain and dysfunction in the jaw joint and the muscles that control jaw movement. We don’t know for certain how many people have TMJ disorders, but some estimates suggest that over 10 million North Americans are affected. The condition appears to be more common in women than men. TMJ is referred to by different names such as TMD, TMJ disorder, and TMJ dysfunction.
For most people, pain in the area of the jaw joint or muscles does not signal a serious problem. Generally, discomfort from these conditions is occasional and temporary, often occurring in cycles. The pain eventually goes away with little or no treatment. Some people, however, develop significant, long-term symptoms.
What is the temporomandibular joint?
The temporomandibular joint connects the lower jaw, called the mandible, to the bone at the side of the head, which is the temporal bone. If you place your fingers just in front of your ears and open your mouth, you can feel the joints. Because these joints are flexible, the jaw can move smoothly up and down and side to side, enabling us to talk, chew, and yawn. Muscles and ligaments attached to and surrounding the jaw joint control its position and movement.
When we open our mouths, the rounded ends of the lower jaw, called condyles, glide along the joint socket of the temporal bone. The condyles slide back to their original position when we close our mouths. To keep this motion smooth, a soft disc lies between the condyle and the temporal bone. This disc absorbs shocks to the jaw joint from chewing and other movements.
The temporomandibular joint is different from the body’s other joints since the joint actually dislocates after opening past a certain point. The combination of hinge and sliding motions makes this joint among the most complicated in the body. Also, the tissues that make up the temporomandibular joint differ from other load-bearing joints, like the knee or hip. Because of its complex movement and unique makeup, the jaw joint and its controlling muscles can pose a tremendous challenge to both patients and health care providers when problems arise.

